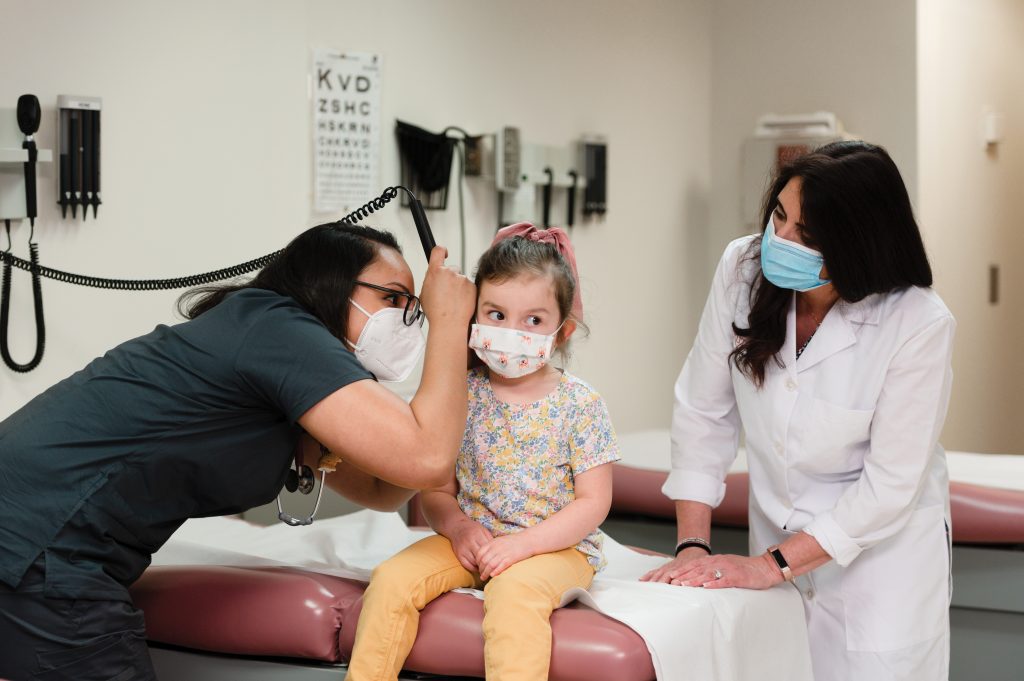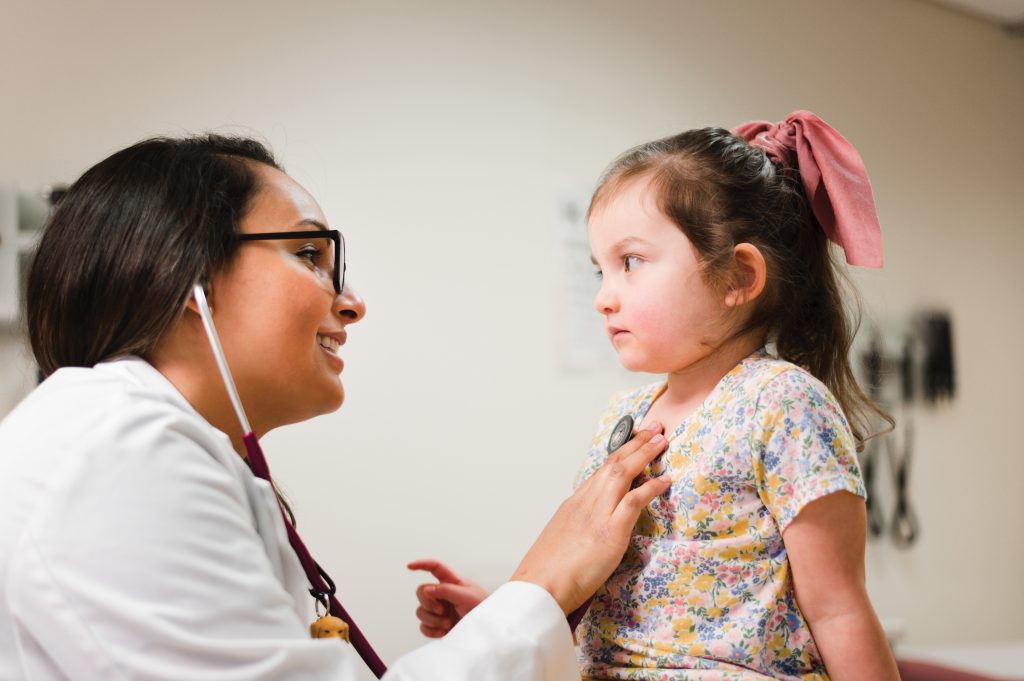
Angela Otto-Ryan (DNP, RN, CBC) was in an enviable position.
Two weeks before her May 2021 graduation from Rutgers School of Nursing’s Primary Care Pediatric Nurse Practitioner program, she was weighing two job offers, both involving work with underserved populations. Over the next decade, her conundrum—choosing among multiple offers of employment—is likely to become increasingly common for pediatric nurse practitioners, or PNPs.
“There is a forecasted critical shortage, over the next 10 years, for PNPs,” says Margaret Quinn, specialty director of the PNP program at Rutgers School of Nursing, “especially in rural and underserved areas.”
The School of Nursing is rising to address that shortage. In addition to its flagship four-year Primary Care PNP program, it also offers a post-master’s certificate in pediatric primary care for nurse practitioners. And this spring, the school launched two new pediatrics programs, a Dual Primary/Acute Care PNP doctor of nursing practice degree—the only one in the state of New Jersey—and a Pediatric Acute Care Post-Master’s Certificate.
Quinn has also been able to secure two grants, one from the Wells Fargo/Edward W. & Stella C. Van Houten Memorial Fund to support scholarships for students in the Pediatric Acute Care Post-Master’s Certificate program and the other, from the New Jersey Health Foundation, to fund the development of a pediatric simulation suite. The suite will offer the first pediatric-sized task trainers at the university and will allow PNP students and others in the School of Nursing to practice highly specialized procedures like spinal taps and umbilical line insertions.
It’s this level of attention to detail that makes the school’s PNP programs so competitive. The flagship primary care PNP program, for instance, offers a comprehensive curriculum comprising health promotion and the treatment of mild, complex, and chronic illnesses among children. It also requires a minimum of 585 clinical hours designed to expose students to a wide variety of clinical settings. (The new dual PNP program, beginning in fall 2021, will require 900 clinical hours.) For Otto-Ryan, who received her accelerated Bachelor of Science in Nursing degree from Rutgers in 2016 and worked as a school nurse and a pediatric surgical nurse before enrolling in the PNP program, the program’s focus on what she calls “the bigger picture” was revelatory. In her previous positions, she says, “there was always such a large emphasis on fixing the problem in front of you.” The PNP program, on the other hand, “was all about prevention and educating patients’ families and promoting health.”

“The focus of a primary care PNP,” says Quinn, “is the outpatient setting: schools, community centers, doctors’ offices, clinics.” The new dual program, she notes, “will open up a whole variety of additional experiences, like inpatient, emergency room, urgent care, and surgical, and it’s also a great crossover for those NPs who want to specialize in areas like cardiology or pulmonology.”
All four programs will prepare students for a changing pediatrics landscape. Today, for instance, 26.6 percent of children suffer from chronic health conditions like asthma, obesity, and ADHD—an increase of more than 100 percent from 12.8 in 1994. On the other hand, fewer children are being treated in hospitals, and the trend toward home care—which requires parent education and dedicated practitioner follow-up—calls for exactly the kind of skills PNPs are trained in.
When Otto-Ryan starts her next job, wherever it may be, she’ll relish the opportunity, she says, to work closely with patients and their families in just this way—to head off the development of chronic conditions and, in her words, “to help children off to a healthy life.”
It’s what Quinn, a PNP herself, has dedicated her career to.
“If we have healthy children,” she stresses, “we’ll have a healthy future.”